What is pelvic floor dysfunction?
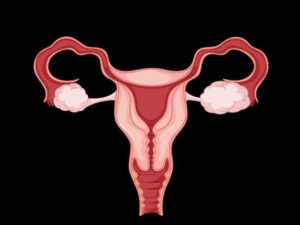
Your pelvic floor is a cluster of muscles and ligaments in your pelvic region. The pelvic floor acts just like a sling to support the organs in your pelvis — bladder, rectum, and female internal reproductive organs. Contraction and relaxation of these muscles permit you to manage your urination, bowel movements, and uterine contractions. The pelvic organs include the bladder, the uterus, and vagina, and the rectum in women. When these muscles are normal you don’t have problems tightening and relaxing pelvic floor muscles.
The inability of the pelvic floor muscles to contract and relax properly may result in pelvic floor dysfunction (PFD). A majority of women with pelvic floor problems may have chronic constipation; urine or stool leakage; frequent urination urge; pain during sexual intercourse, and problems controlling bowel movements. Some women may also face symptoms like abdominal pain and bloating.
Pelvic Floor Dysfunction Symptoms
If left untreated, the condition will result in discomfort, colon problems, or infection. There are a variety of symptoms related to pelvic floor problems. If you’re diagnosed with pelvic floor dysfunction, you will experience symptoms like:
- Urinary problems, like the urge to urinate or painful voiding
- Constipation or abdominal cramps
- Lower back pain
- Pain within the pelvic region, genitals, or rectum
- Pressure within the pelvic region
- Muscle spasms within the pelvis
- Unexplained lower back pain
- Painful urination
- Urinary or fecal incontinence
- Persistent pain in the rectum, genitals, and pelvic region – with or without bowel movements.
What are the causes of pelvic floor dysfunction?
The causes of pelvic floor dysfunction are still unknown. But experts link pelvic floor dysfunction to conditions that weaken the pelvic muscles or the connective tissue – including:
- Nerve damage
- Injuries to the pelvic region
- Pushing muscles too hard due to constipation
- Overuse of pelvic muscles
- Obesity
- Childbirth
- Advancing age
- Pelvic surgery
Diagnosis
It is very important not to self-diagnose your symptoms because doing so might lead to unhealthy consequences.
Your gynecologist who specializes in urogynaecology asks you about the symptoms and takes note of your medical history. She will ask you a few questions related to your pregnancy and childbirth. She will also ask whether you have pain during sex; bladder inflammation or irritable bowel syndrome and whether you strain during a bowel movement. She will do a physical examination to check how well you control your pelvic floor muscles and recommend rectal and vaginal exams.
An internal exam is performed by your doctor by placing a perineometer (a small, sensing device into your rectum or vagina) to check pelvic muscle control and pelvic muscle contractions.
Anorectal manometry: This test helps in measuring the strength and working ability of anal sphincters – to check the pressure, muscle strength, and coordination.
A uroflow test help in determining how well you can empty your bladder. A weak urine flow and if you stop and start when you urinate can signal pelvic floor dysfunction.
What is the treatment for pelvic floor dysfunction?
Treatment for pelvic floor dysfunction is required to relax the pelvic floor muscles and to make bowel movements easier. There are different types of approaches to treating the condition. Initial treatments include biofeedback, pelvic floor exercises, physical therapy, and medications.
In a majority of cases, the condition is treated without surgery. Non-surgical options include the following:
Physical therapy: Physical therapist will train the affected muscles of the pelvic floor. After determining which muscles need training, the physiotherapist teaches a few exercises to stretch those muscles to improve their flexibility, strength, and endurance and to improve their coordination.
Biofeedback: In this technique, your physiotherapist uses special sensors and videos to monitor your pelvic floor muscles when you stretch and relax them. The physiotherapist then gives you feedback and works with you to improve your muscle coordination. This technique helps a majority of people with pelvic floor dysfunction.
Pelvic floor dysfunction exercises
Relaxation methods: Yoga, acupuncture, warm baths, meditation, and other exercises will help you relax holistically. You can work with a special trainer – who will guide you properly in these techniques. Kegel exercises that require the contraction of muscles will help in specific cases of incontinence.
Talk to your gynecologist about dietary modifications and other lifestyle changes to manage this condition.
Medication – you must follow the prescription prescribed by the doctor.
When is Surgery Required for Pelvic floor dysfunction?
When prolapse interferes with daily activities, your gynecologist may recommend surgery. If you have any concerns pertaining to the symptoms associated with your pelvic floor muscles, call and fix an appointment for further discussion.